- Category: IV Therapy
Migraine IV Treatment: The Cocktail Approach to Acute Migraine Relief
Share on:
Why oral migraine medications often fail during an active attack
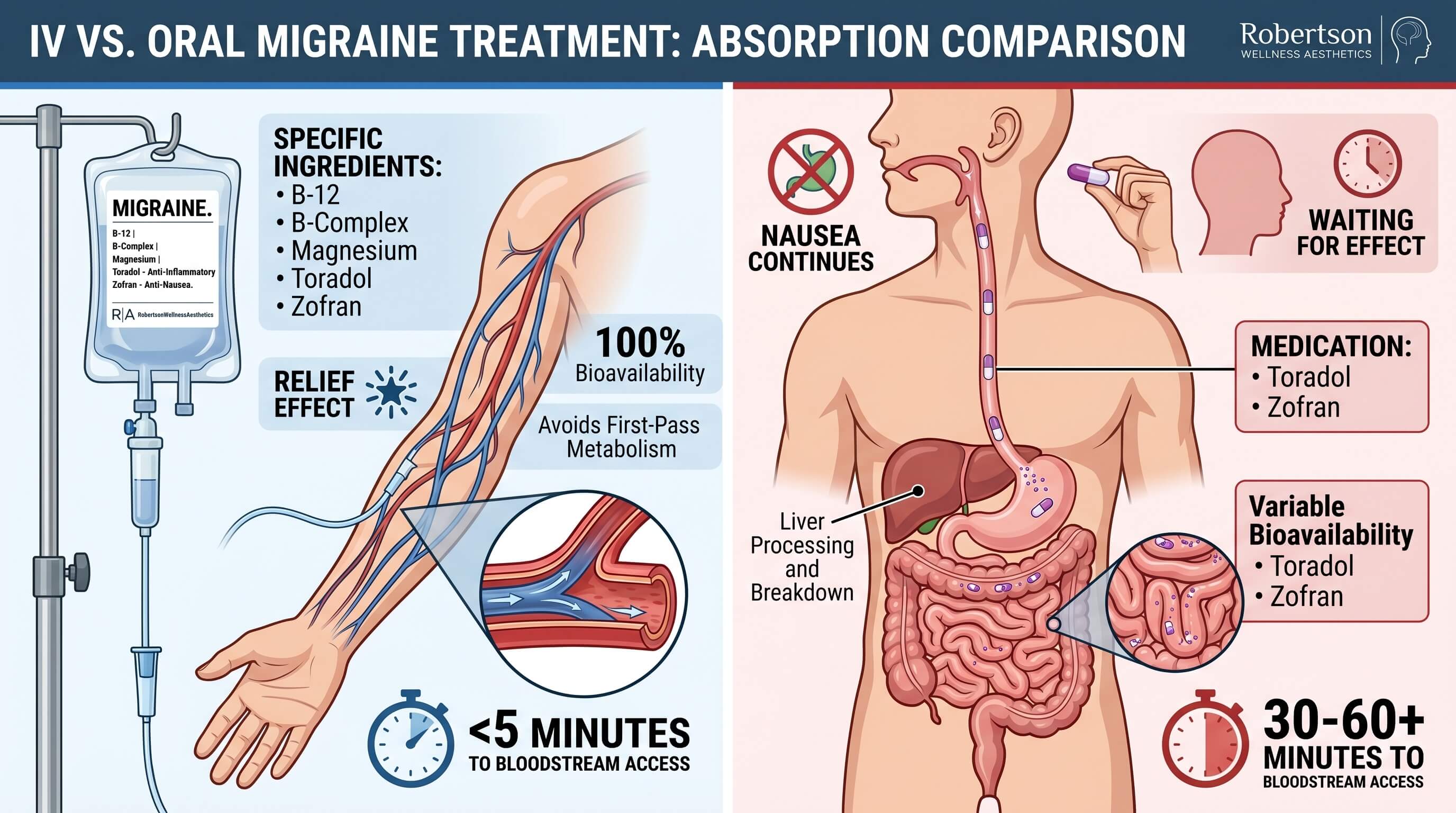 Most people try oral medications first when a migraine begins. For mild to moderate attacks, this approach works reasonably well. For severe attacks, and particularly for attacks that have progressed past the early stage, oral options frequently fall short. Understanding why helps explain the rationale for IV therapy.
Gastric stasis: During a migraine attack, the stomach’s normal motility slows down. This is well-documented in migraine research and is part of the reason why nausea is such a common companion to migraine pain. When the stomach is not emptying normally, oral medications sit there rather than reaching the small intestine, where absorption occurs.
Nausea and vomiting: When an attack is severe enough to cause vomiting, oral medications may be expelled before they have a chance to work. Even without vomiting, the nausea itself discourages patients from taking or keeping down tablets.
Delayed absorption and peak levels: Even in patients who can tolerate oral medication, absorption during an active migraine is typically slower than usual. By the time serum levels peak, the attack may have progressed.
Medication-overuse concerns: Patients who experience frequent severe attacks often find themselves taking multiple oral doses during a single episode, which raises the risk of medication-overuse headache over time.
Intravenous delivery bypasses all of these barriers. Medications reach the bloodstream directly, fluid and electrolyte status can be addressed simultaneously, and multiple therapeutic mechanisms can be combined into one session. This is why emergency departments and specialty clinics have developed standardized IV protocols for severe migraine.
Most people try oral medications first when a migraine begins. For mild to moderate attacks, this approach works reasonably well. For severe attacks, and particularly for attacks that have progressed past the early stage, oral options frequently fall short. Understanding why helps explain the rationale for IV therapy.
Gastric stasis: During a migraine attack, the stomach’s normal motility slows down. This is well-documented in migraine research and is part of the reason why nausea is such a common companion to migraine pain. When the stomach is not emptying normally, oral medications sit there rather than reaching the small intestine, where absorption occurs.
Nausea and vomiting: When an attack is severe enough to cause vomiting, oral medications may be expelled before they have a chance to work. Even without vomiting, the nausea itself discourages patients from taking or keeping down tablets.
Delayed absorption and peak levels: Even in patients who can tolerate oral medication, absorption during an active migraine is typically slower than usual. By the time serum levels peak, the attack may have progressed.
Medication-overuse concerns: Patients who experience frequent severe attacks often find themselves taking multiple oral doses during a single episode, which raises the risk of medication-overuse headache over time.
Intravenous delivery bypasses all of these barriers. Medications reach the bloodstream directly, fluid and electrolyte status can be addressed simultaneously, and multiple therapeutic mechanisms can be combined into one session. This is why emergency departments and specialty clinics have developed standardized IV protocols for severe migraine.
What “migraine IV cocktail” actually means
The term “migraine cocktail” refers to a combination of intravenous medications and fluids given together during a single session. The rationale is straightforward: migraine is a complex neurological event that involves pain pathways, inflammation, dopamine signaling, nausea circuits, and often fluid imbalance. A single-medication approach addresses only one aspect. A combination approach targets several mechanisms at once. At Robertson Wellness Aesthetics in Beverly Hills, our migraine IV cocktail is designed around the same evidence-based principles used in emergency department and neurology clinic protocols, with every session overseen by a licensed medical professional. This is distinct from general wellness IV options such as the Myers cocktail or an energy boost IV, which serve different purposes. It is important to note that IV migraine treatment is intended as an acute intervention during a severe attack or a medical visit for recurrent migraine management, not as a daily therapy. Chronic migraine management typically requires a broader plan developed with a neurologist or headache specialist.Common ingredients in a migraine IV cocktail
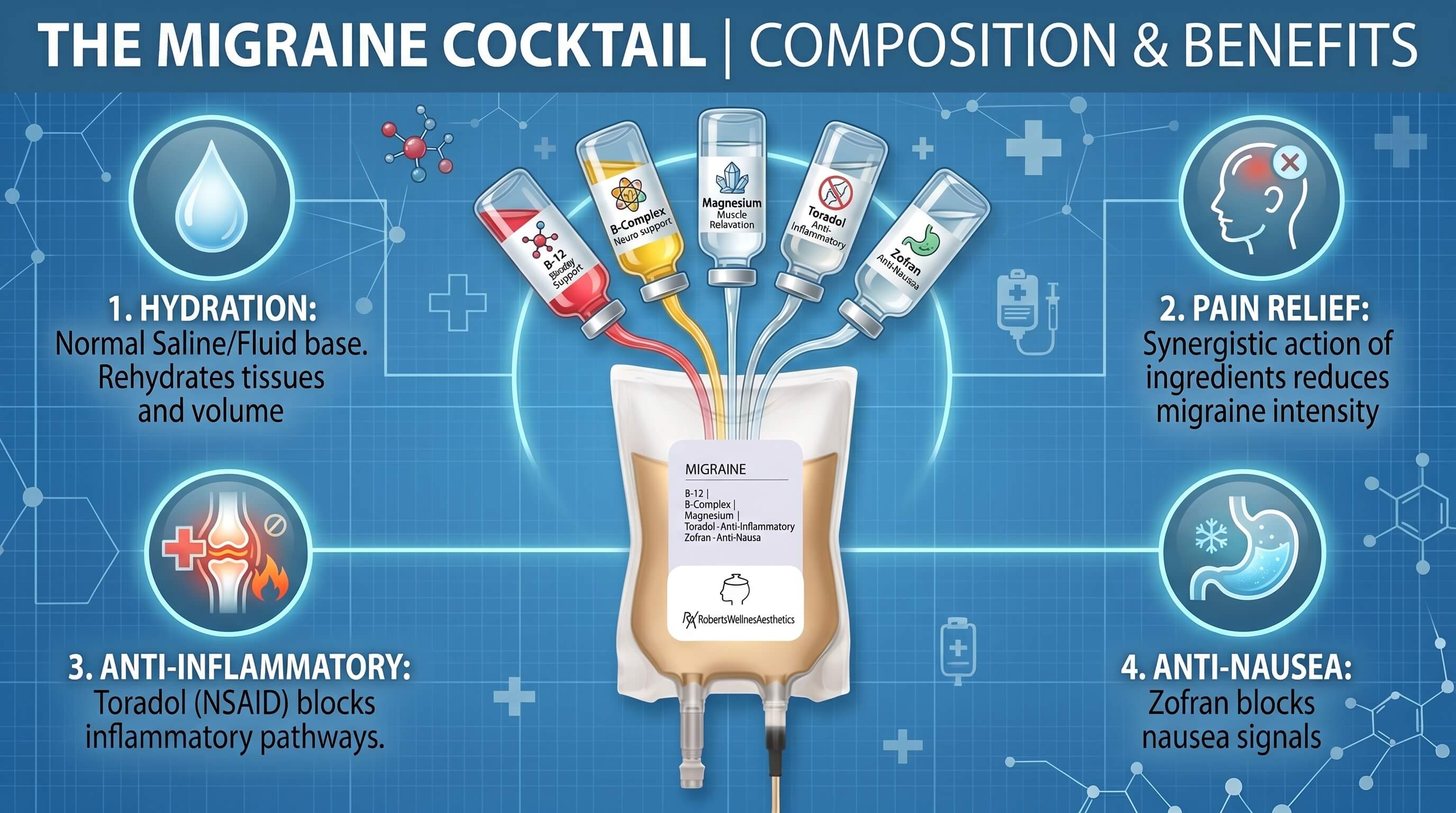 The exact formulation varies based on clinical protocol, patient history, and provider judgment. The table below summarizes the most commonly used medications and their associated roles.
The exact formulation varies based on clinical protocol, patient history, and provider judgment. The table below summarizes the most commonly used medications and their associated roles.
| Component | Typical IV dose | Role in migraine protocols |
|---|---|---|
| Normal saline (IV fluids) | 1 liter | Addresses dehydration, supports blood pressure during medication administration |
| Ketorolac (Toradol) | 15 to 30 mg | NSAIDs that plays a role in reducing inflammation-related pain signaling |
| Metoclopramide (Reglan) | 10 mg | An antemetic that is being studied for its dual role in the nausea and migraine pathways |
| Prochlorperazine (Compazine) | 10 mg | Antiemetic with dopamine receptor activity, often used in emergency migraine protocols |
| Diphenhydramine (Benadryl) | 25 to 50 mg | Often added to reduce the risk of restlessness associated with dopamine-blocking antiemetics |
| Magnesium sulfate | 1 to 2 g | Being studied for its role in migraine, particularly migraine with aura |
| Dexamethasone | 4 to 10 mg | A corticosteroid that has been studied for reducing headache recurrence in the 24 to 72 hours after treatment |
Why each component is used
IV fluids and hydration
Dehydration is widely considered a migraine trigger, and nausea or vomiting during an attack can worsen fluid loss. IV fluids address volume status directly. Beyond addressing dehydration, fluids also help prevent the postural lightheadedness that can accompany some of the other medications used in migraine protocols. Adequate hydration is also thought to provide some renal protection when NSAIDs like ketorolac are used.Ketorolac and NSAIDs
Ketorolac is the injectable NSAID most commonly used in US emergency departments for acute migraine. Randomized studies have supported its use as monotherapy in appropriate patients, and it is often included as part of combination protocols. NSAIDs play a role in reducing the inflammatory signaling involved in migraine pain pathways. Ketorolac is not appropriate for everyone. Patients with active peptic ulcer disease, significant kidney disease, bleeding disorders, or certain cardiovascular conditions may need alternatives.Dopamine receptor antagonists (metoclopramide, prochlorperazine)
These medications were originally developed as antiemetics, but clinical research has shown that they have migraine-specific effects independent of their anti-nausea properties. Both have been evaluated in randomized controlled trials for acute migraine, and both carry formal recommendations in headache treatment guidelines. Prochlorperazine has been rated slightly higher in some guideline reviews, while metoclopramide remains widely used and effective. These medications can cause a restless sensation called akathisia in a small percentage of patients, which is why diphenhydramine is often given alongside them as a preventive measure.Diphenhydramine
Diphenhydramine serves two functions in a migraine cocktail. First, it may reduce the risk of akathisia from dopamine-blocking antiemetics. Second, some evidence suggests it may have modest direct effects on migraine symptoms, though data here are limited. Because it commonly causes drowsiness, patients should plan for transportation after a session.Magnesium
Intravenous magnesium is being studied for its role in migraine, with the strongest evidence in patients with migraine with aura. It is often included when an aura is present or when a patient has a history suggesting magnesium responsiveness. Hypotension is a known side effect, which is part of why IV fluids are typically given alongside or before magnesium administration.Dexamethasone
Dexamethasone is a corticosteroid that has been studied specifically for preventing migraine recurrence in the 24 to 72 hours after the initial treatment. It is not primarily used to abort the current migraine, but rather to reduce the chance that the attack returns shortly after the initial relief. A single IV dose of 10 mg, or repeated smaller doses, is a common approach.What a migraine IV session feels like
Most patients are curious about what to expect, particularly if they have only received migraine treatment in an emergency room before. Here is a realistic walkthrough of a clinic-based session. Before the session: You will complete an intake form covering medical history, current medications, allergies, migraine history, and what has already been tried during the current attack. A qualified provider reviews the information. If you have kidney disease, active peptic ulcer disease, certain cardiac conditions, or take medications that interact with common migraine cocktail components, the provider may modify the protocol or decline specific ingredients. Setup: A licensed medical professional checks your vital signs, examines your veins, and places a small IV catheter, usually in the forearm or hand. Placement feels like a brief pinch. Lighting and noise are typically kept low, recognizing that both are common migraine triggers. During the infusion: The session typically lasts 45 to 90 minutes, depending on which components are included and how they are infused. Fluids run continuously. Medications are usually given as slow pushes or short infusions. Some patients report noticing relief within the first 20 to 30 minutes; others take longer. A brief sensation of warmth, a mild metallic taste, or drowsiness are all common. After the infusion: The catheter is removed and a small bandage applied. Because diphenhydramine and some of the antiemetics cause drowsiness, patients are often advised to arrange transportation home and to rest for the remainder of the day. Some report that their migraine returns within 24 to 72 hours, which is part of why dexamethasone is sometimes included. Others experience sustained relief. Individual results vary.Clinic-based IV therapy compared to the emergency room
Patients who deal with severe recurrent migraines often face a difficult choice when an attack escalates: endure it at home, or go to the emergency room. Both options have limitations. The table below outlines how clinic-based IV therapy compares.| Factor | Emergency department | Clinic-based IV therapy |
|---|---|---|
| Availability | 24 hours | Business hours, by appointment |
| Wait time | Often several hours | Short, scheduled |
| Environment | Bright lights, noise, a busy setting | Quiet, controlled environment |
| Medical oversight | ER physicians and nurses | Licensed medical providers with clinic protocols |
| Appropriate for | Suspected serious causes, neurologic red flags, severe vomiting, pregnancy | Known migraine, stable patient, recurrent attacks |
| Cost | Often high, variable insurance coverage | Typically out-of-pocket, predictable pricing |
| Follow-up | Limited, typically a single visit | Can be integrated into ongoing wellness planning |
Who may be a candidate for migraine IV therapy
Populations who often explore migraine IV treatment include:- Adults with a confirmed migraine diagnosis who have had severe attacks before and know their pattern
- Patients whose oral medications have become less effective during active attacks
- Individuals dealing with medication-overuse headache concerns who are working to reduce oral medication frequency
- Patients in the recovery phase after a severe migraine who are at risk of recurrence
- Frequent migraine sufferers looking for an alternative to repeated ER visits for typical attacks
- Anyone with a first-time severe headache or a headache that differs from their typical pattern
- Pregnant or breastfeeding women, for whom many cocktail components are contraindicated or require alternatives
- Patients with kidney disease (relevant for NSAIDs)
- Patients with significant cardiovascular disease (relevant for several components)
- Patients with active peptic ulcer disease (relevant for NSAIDs)
- Patients with known Parkinson’s disease or movement disorders (relevant for dopamine antagonists)
- Patients with certain cardiac arrhythmias or QT prolongation (relevant for some antiemetics)
- Anyone with allergies to common cocktail components
Potential side effects and safety considerations
When administered by a qualified medical professional using proper protocols, a migraine IV cocktail has a reasonable safety profile, but no medication is without potential side effects. Commonly reported effects include:- Drowsiness, particularly from diphenhydramine and some antiemetics
- Restlessness or akathisia, typically transient and often prevented by diphenhydramine pretreatment
- Mild lightheadedness, particularly when standing up after a session
- A warming sensation or flushing during magnesium administration
- A brief metallic or medication taste during infusion
- Bruising or tenderness at the IV site
- Rarely, allergic reactions to specific components
How often can migraine IV therapy be used?
There is no one-size-fits-all answer. For many patients, IV therapy is used occasionally, for severe breakthrough attacks or for attacks that have not responded to their usual abortive medications. For others, a scheduled approach during a predictable severe attack period may make sense.| Usage pattern | Typical frequency | Typical context |
|---|---|---|
| As-needed for severe attacks | Once per attack, occasional | Typical severe migraine that does not respond to oral medication |
| Short series | 1 to 3 sessions over a few days | Status migrainosus or protracted attack |
| Preventive support | Variable, as part of a broader plan | Integrated with neurologist-managed migraine care |
Migraine IV therapy in the context of broader wellness
Migraine is a neurological condition, not simply a bad headache, and effective long-term management usually requires more than acute interventions alone. IV therapy addresses active attacks but does not replace preventive care. Many patients integrating IV therapy into their migraine management also use other supportive wellness approaches. Some find that Myers cocktail IV therapy at regular intervals supports general wellness and may help with metabolic support, though this is separate from acute migraine treatment. Others address hydration concerns with IV hydration therapy, recognizing that dehydration is a common trigger. The foundations of migraine management remain the same evidence-based basics recognized across neurology: regular sleep patterns, adequate hydration, consistent meal timing, trigger identification, stress management, and preventive medications where appropriate. IV acute treatment is a valuable tool, but it is most effective as part of a broader plan. Some patients also explore complementary approaches such as peptide therapy in consultation with their provider.Frequently asked questions
How quickly does a migraine IV cocktail work? Some patients report noticing improvement within 20 to 30 minutes of starting the infusion. Others take longer. Individual results vary. Will the migraine come back? Some patients experience recurrence within 24 to 72 hours. This is part of why dexamethasone is sometimes included in cocktails, as it has been studied for reducing recurrence. Can I drive after a session? Most patients should not drive after a migraine IV session because of drowsiness from diphenhydramine and antiemetics. Arrange transportation in advance. Is migraine IV therapy FDA-approved? The individual medications used are FDA-approved, though specific uses within a migraine cocktail may be off-label. The combination itself as a “migraine cocktail” is a clinical protocol developed through decades of practice, not a single approved formulation. Does insurance cover clinic-based migraine IV therapy? Coverage varies. Many wellness-focused IV therapy clinics operate on an out-of-pocket basis. Emergency department IV treatment is typically processed through insurance but carries its own cost and time burden. Is this the same as the Raskin protocol? No. The Raskin protocol is a multi-day inpatient DHE-based regimen for refractory migraine. Clinic-based IV cocktails are single-session outpatient treatments using a different combination of medications. Can IV therapy replace my preventive migraine medications? No. IV therapy is an acute treatment, not a substitute for preventive care. Patients with frequent severe attacks should work with a neurologist or headache specialist on a comprehensive plan.Ready to learn whether migraine IV treatment is right for you?
At RWA Center in Beverly Hills, our medical team offers migraine IV cocktail therapy as part of a broader menu of IV treatments, with every session overseen by licensed medical professionals. Each protocol is personalized based on a consultation covering your migraine history, current medications, and overall health picture. If you are exploring IV therapy for the first time or looking for an alternative to emergency department visits for severe attacks, we invite you to contact our team to discuss whether this approach is appropriate for your situation. The information provided is for educational purposes only and is not intended as medical advice. Certain therapies discussed may be investigational and are not approved by the FDA for the diagnosis, treatment, cure, or prevention of disease. Always consult with a qualified healthcare professional before beginning any new wellness protocol.Request a Consultation
Recommended for you

How Much Does UBI Treatment Cost?
If you are researching ultraviolet blood irradiation (UBI), one of the first questions is usually cost. This guide gives you clear, current 2026 pricing at Robertson Wellness and Aesthetics in

Does UBI Therapy Really Work?
Ultraviolet blood irradiation (UBI) is one of the older therapies in integrative medicine, with origins in the 1940s and a recent resurgence of interest. If you are researching whether it

Peptides for weight loss: a physician’s guide to what’s being studied
Medically reviewed by Biana Borchenko, FNP-BC | Robertson Wellness and Aesthetics, Beverly Hills Weight loss is one of the most active areas of peptide research today. Some peptide-based medications, like

Does Ozone Therapy Hurt? An Honest Answer About Pain, Comfort, and Side Effects
Most patients describe ozone therapy as comfortable, not painful. The only consistent moment of mild discomfort is the initial IV placement – the same brief pinch you would feel with

Best Peptides for Brain Fog: Beverly Hills Guide 2026
You finish a meeting and cannot remember what was decided. You walk into a room and forget why. You read the same paragraph three times. The word you need sits

NAD+ IV Therapy: What to Expect Before, During & After
Most patients booking NAD+ IV therapy at Robertson Wellness and Aesthetics have the same set of questions in the days before their first infusion. What does it actually feel like?

